AI in PHI Classification: Benefits and Risks
Post Summary
AI tools are transforming how Protected Health Information (PHI) is classified. By using Natural Language Processing (NLP) and machine learning, these tools can quickly and accurately identify sensitive data across structured and unstructured sources. This technology reduces manual review times by up to 85% and achieves over 90% precision in detecting PHI. However, AI systems come with risks like re-identification and potential data exposure, making governance essential. Platforms like Censinet RiskOps™ combine AI automation with human oversight to manage these risks effectively while ensuring compliance with regulations like HIPAA. Balancing efficiency with security is key to successful PHI management.
Residual PHI Risk in Clinical NLP: Why High F1 Scores Still Fail HIPAA Compliance
sbb-itb-535baee
1. AI-Driven PHI Classification Tools
Modern AI tools for Protected Health Information (PHI) classification go beyond simple keyword searches - they grasp the full context. By using Natural Language Processing (NLP), machine learning, and entity recognition, these tools can analyze both structured data and unstructured sources, such as clinician notes, scanned documents, and communication logs. This approach brings a new level of efficiency to the process.
Efficiency in PHI Identification
The results speak for themselves. For instance, one healthcare provider managed to narrow down 3.8 million potentially sensitive documents to just 20,000 by using AI tools [3]. This drastic reduction minimizes the need for manual review and focuses attention on the most critical documents.
"AI solutions leverage advanced techniques like Natural Language Processing (NLP), machine learning, and entity recognition to detect sensitive information with greater precision." - Ankura [3]
Once PHI is identified, automated labeling ensures that persistent tags are applied to the data. These tags enable downstream systems - like encryption tools, access controls, and Data Loss Prevention (DLP) platforms - to take action automatically.
Accuracy and Risk Mitigation
AI tools don't just work faster; they work smarter. They enhance accuracy by understanding the relationships between data points rather than relying solely on pattern matching. For example, a medication name that coincidentally matches a person's name wouldn't be flagged as PHI, but a patient's name paired with a lab result would. These tools are trained to make such distinctions and can also handle complex formats. Optical Character Recognition (OCR) processes PDFs and faxes, while machine learning models analyze diagnostic images and screenshots.
Risk mitigation doesn't stop at detection. Some AI tools offer inline remediation, which allows them to redact, mask, or block PHI before it can appear in SaaS applications, cloud drives, or even within a GenAI prompt. Additionally, techniques like k-anonymity are applied to free-text clinical notes to prevent re-identification [1].
Governance and Compliance Features
Precise classification plays a key role in meeting HIPAA requirements. AI tools use their context-aware accuracy to ensure that PHI is accessible only to authorized personnel. They align with HIPAA's "minimum necessary" standard by linking classification labels to role-based access controls. Predefined templates, designed to recognize HIPAA identifiers like Social Security numbers, medical record numbers, and ICD codes, simplify the configuration process and reduce manual work.
Real-time audit trails further bolster compliance by logging every interaction with PHI, providing a clear record of due diligence for regulatory investigations. As PHI definitions expand to include genomic data and medical device identifiers, classification engines are adapting by training on increasingly diverse datasets.
"Protected Health Information (PHI) is some of the most sensitive data an organization can hold, and it's also some of the most complex to classify." - Tom Mayblum, VP of Product, MIND [4]
2. Censinet RiskOps™ with AI Capabilities
Censinet RiskOps™ takes AI's ability to efficiently classify Protected Health Information (PHI) and applies it to the broader challenge of risk management. Unlike standalone AI tools that focus solely on tagging sensitive data, Censinet RiskOps™ integrates AI throughout the entire PHI risk management process. For healthcare delivery organizations (HDOs) and their vendors, this approach is critical. Managing PHI risk isn't just about identifying sensitive data - it’s about knowing who interacts with it, how it’s handled, and whether safeguards are in place.
Efficiency in PHI Identification
Censinet RiskOps™ streamlines PHI identification by standardizing how vendors and internal teams report on sensitive data practices. The platform centralizes vendor intake by immediately gathering details like business associate status, PHI storage practices, transmission methods, and de-identification procedures. This eliminates the back-and-forth typically associated with emails or spreadsheets.
Censinet AI™ takes this a step further, enabling vendors to complete security questionnaires in seconds and automatically summarizing their evidence and documentation [7]. According to Censinet, health systems leveraging RiskOps have reduced third-party risk assessment timelines by over 50%, cutting processes that once took months down to just weeks - or even less [7].
Accuracy and Risk Mitigation
Effective PHI risk management goes beyond detection; it requires consistency in evaluation. Censinet RiskOps™ ensures this by applying standardized control sets to every vendor review, minimizing variability. The platform’s risk scoring dashboards identify specific control weaknesses - like missing multi-factor authentication, incomplete encryption, or inadequate incident response plans - allowing security teams to prioritize the most pressing risks.
Remediation tasks are tracked to completion, and re-assessments are built into the workflow to ensure ongoing risk reduction [6]. While Censinet AI automates routine tasks, final decisions on complex or high-stakes issues are made by trained risk teams using configurable review rules. This human oversight is essential in compliance-heavy settings, where errors could lead to privacy breaches or contractual violations.
Governance and Compliance Features
Censinet RiskOps™ aligns vendor assessments directly with regulatory frameworks like the HIPAA Security Rule, NIST CSF, and HICP. This gives compliance teams clear insight into how vendor responses meet regulatory requirements [6]. Features like audit-ready exports, centralized sign-offs, and role-based collaboration across departments - including security, legal, procurement, and clinical operations - ensure that every PHI-related decision is documented.
A survey sponsored by Censinet and the American Hospital Association revealed that 61% of health systems feel they lack adequate resources to manage third-party and enterprise cyber risks effectively [7]. By addressing these challenges, Censinet RiskOps™ offers a practical solution for improving governance and compliance in the healthcare sector.
Pros and Cons
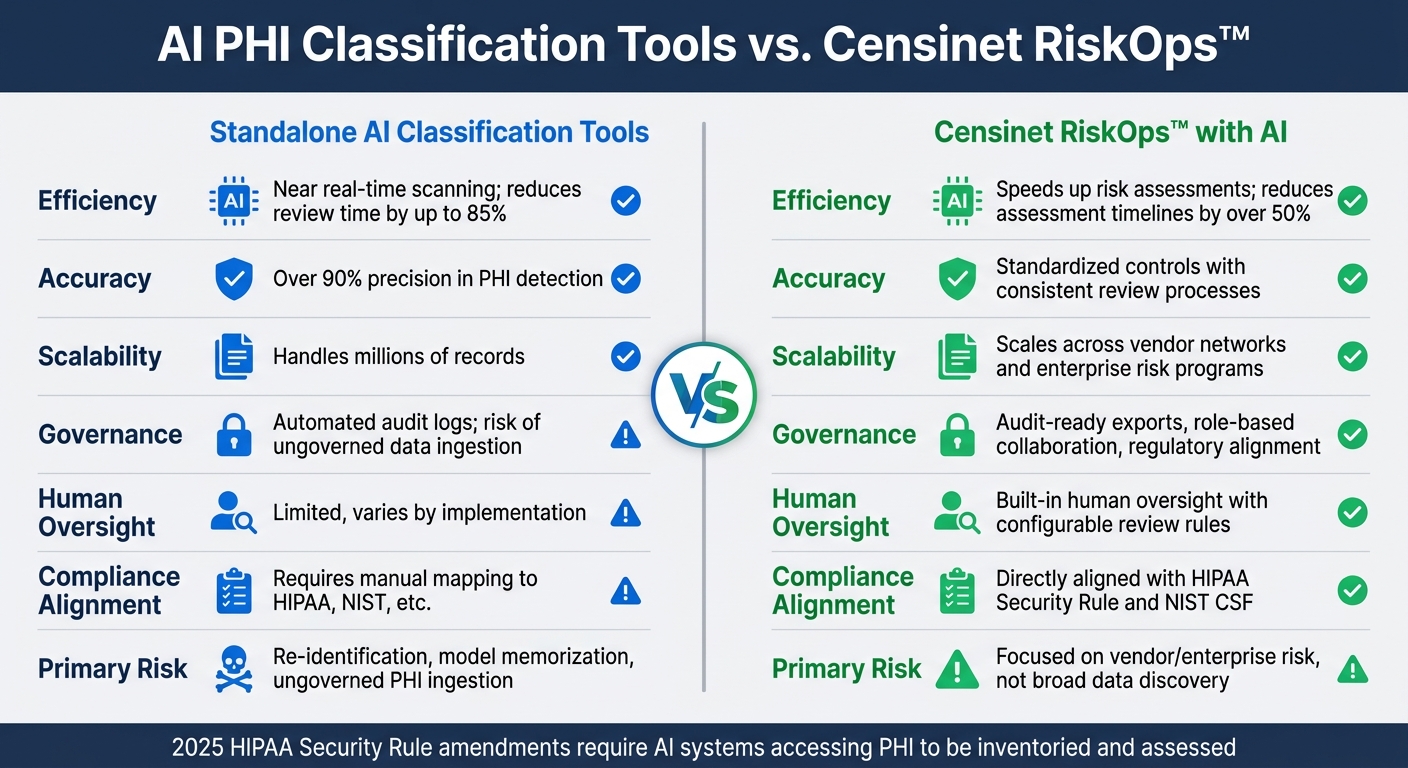
AI PHI Classification Tools vs. Censinet RiskOps™: Feature Comparison
Building on the capabilities outlined earlier, let’s examine the benefits and challenges of each approach.
Standalone AI-driven PHI classification tools and integrated platforms like Censinet RiskOps™ each offer their own strengths and limitations.
AI-driven tools excel at processing massive datasets, scanning millions of records in near real-time. They can reduce review times by up to 85% while maintaining over 90% precision in detecting PHI [3]. However, these tools come with risks. For example, Large Language Models (LLMs) might inadvertently expose training data. Additionally, AI-generated identifiers - like fabricated Social Security Numbers - can trigger forensic audits, even when no actual breach has occurred. Another concern is that clinical narratives may still contain enough context to re-identify patients, even after removing direct identifiers.
"Once PHI enters an AI system without control, reversing exposure is significantly harder than preventing it." - BeKey [1]
Censinet RiskOps™, on the other hand, addresses many of these risks by integrating human oversight into its workflow. The platform allows risk teams to maintain control through configurable review rules. Routine tasks, such as automating questionnaires or summarizing evidence, are handled by Censinet AI™, while complex decisions remain with trained reviewers. The trade-off? RiskOps™ is specialized for third-party and enterprise risk management, making it less suited for large-scale scanning of unstructured data repositories.
Here’s a side-by-side comparison of key features for PHI governance between standalone AI tools and Censinet RiskOps™:
| Feature | Standalone AI Classification Tools | Censinet RiskOps™ with AI |
|---|---|---|
| Efficiency | Near real-time scanning; reduces review time by up to 85% [3] | Speeds up risk assessments through streamlined workflows |
| Accuracy | Over 90% precision in PHI detection [3] | Standardized controls with consistent review processes |
| Scalability | Handles millions of records | Scales across vendor networks and enterprise risk programs |
| Governance | Automated audit logs; some risk of ungoverned data ingestion | Audit-ready exports, role-based collaboration, and regulatory alignment |
| Human Oversight | Limited and varies by implementation | Built-in human oversight with configurable review rules |
| Compliance Alignment | Requires manual mapping to HIPAA, NIST, etc. | Directly aligned with HIPAA Security Rule and NIST CSF |
| Primary Risk | Re-identification, model memorization, and ungoverned PHI ingestion | Focuses on vendor and enterprise risk, not broad data discovery |
A key point to consider: the upcoming 2025 HIPAA Security Rule amendments mandate that risk analyses must inventory and assess AI systems accessing PHI. This means undocumented AI deployments could be flagged during audits [2]. Both approaches must prioritize robust governance to meet these heightened requirements.
Conclusion
Looking at how AI tools and integrated risk management work together with Censinet RiskOps™, it's clear that the future of PHI classification calls for a well-rounded approach. AI has proven its worth in healthcare data governance, achieving over 90% accuracy in PHI detection and cutting document review times by as much as 85% [3].
But it’s not all smooth sailing. While AI offers incredible efficiency, challenges like re-identification risks and data memorization demand careful human oversight. The 2019 breach at the American Medical Collection Agency, which compromised at least 21 million patient records, is a sobering example of what can go wrong when vendor relationships aren’t tightly managed [5].
The sweet spot lies in combining AI automation with proactive human oversight. AI classification tools excel at processing unstructured data quickly and at scale. Tools like Censinet RiskOps™ take this a step further by integrating human oversight, audit-ready workflows, and regulatory safeguards into the process. This ensures PHI governance extends beyond just detection.
With HIPAA and other regulations evolving, deploying AI without a clear governance framework can quickly turn into a compliance nightmare. A phased approach, centered on governance, is the smartest way to navigate these challenges.
"True success requires a comprehensive strategy that includes governance, policy alignment, and collaboration across legal, privacy, and IT teams." - Ankura [3]
FAQs
What data sources can AI scan for PHI?
AI tools can sift through a wide range of data sources to pinpoint and categorize Protected Health Information (PHI). These sources include electronic health records (EHRs), databases, cloud storage, and other digital repositories. Using machine learning, these systems analyze data in real-time to ensure sensitive information is accurately identified and safeguarded. Beyond that, they keep an eye on older legacy systems and data-sharing activities, helping healthcare organizations stay compliant and minimize the chances of PHI breaches.
How can we prevent re-identification when using AI?
Protecting patient privacy in healthcare while using AI requires strong de-identification strategies that align with HIPAA regulations. Two commonly used methods are:
- Safe Harbor: This involves removing 18 specific identifiers, such as names, Social Security numbers, and addresses, to ensure data cannot be traced back to individuals.
- Expert Determination: This method uses advanced techniques like k-anonymity (grouping data to make individuals indistinguishable) or differential privacy (adding noise to data to obscure individual identities).
Beyond these, additional measures are crucial to maintain privacy. These include:
- Data masking: Obscuring sensitive information to limit access.
- Encryption: Protecting data during storage and transmission.
- Strict access controls: Ensuring only authorized personnel can access sensitive data.
- Regular privacy assessments: Continuously evaluating and improving data protection measures.
Platforms like Censinet RiskOps™ play a key role by centralizing risk management tasks and automating compliance checks. This allows healthcare organizations to balance privacy concerns with the effective use of AI technologies.
What governance is needed for AI that touches PHI?
Managing AI systems that deal with Protected Health Information (PHI) demands strict adherence to HIPAA regulations and a proactive approach to minimizing risks. A key strategy is adopting a "compliance-by-design" framework, where security and legal standards are baked into the system from the ground up.
Some essential practices include:
- Encryption: Safeguarding sensitive data through robust encryption methods.
- Audit Logging: Keeping detailed logs to track system activities and ensure accountability.
- Access Policies: Establishing clear rules about who can access PHI and under what circumstances.
- Defined User Roles: Assigning specific permissions based on roles to limit unnecessary data exposure.
Beyond these foundational measures, ongoing efforts like regular risk assessments, privacy evaluations, and real-time system monitoring are critical to maintaining PHI security. Tools such as Censinet RiskOps™ can streamline this process by offering centralized oversight and automating compliance checks, helping organizations stay on top of their obligations efficiently.


