5 Best Practices for Post-Incident Communication in Healthcare
Post Summary
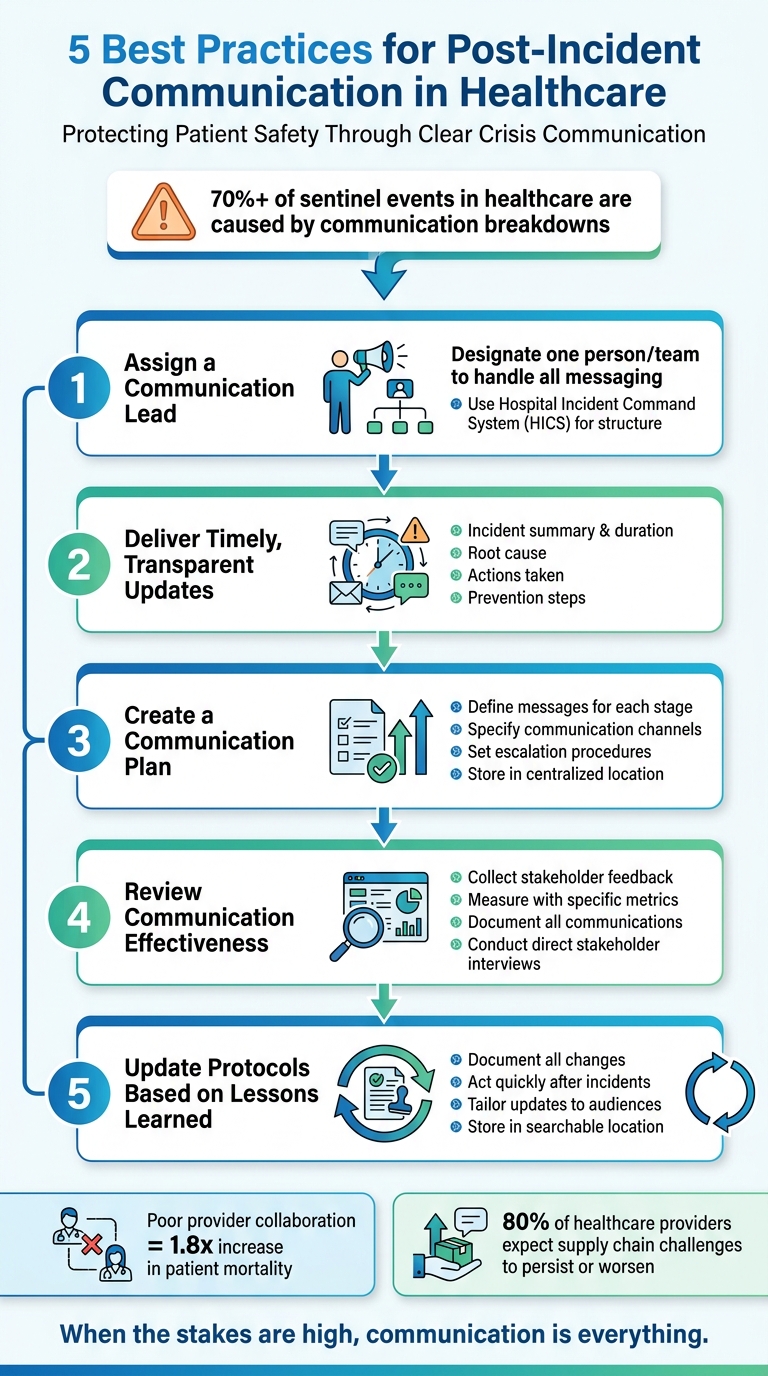
Clear communication after a healthcare incident can save lives and preserve trust. When supply chain issues disrupt patient care or expose sensitive data, how you respond matters. Miscommunication can lead to delays, safety risks, or even higher mortality rates. Here's how to ensure your post-incident communication is effective:
- Assign a Communication Lead: Designate one person or team to handle messaging and avoid confusion.
- Provide Timely Updates: Share consistent, transparent updates with all stakeholders, tailored to their needs.
- Create a Communication Plan: Document roles, escalation procedures, and messaging templates to streamline responses.
- Evaluate Performance: After resolving the issue, review what worked and what didn’t to improve future efforts.
- Update Protocols: Use lessons learned to refine communication processes and prevent repeat mistakes.
Each of these steps helps build trust and ensures smoother recovery during crises. Strong communication isn't just about managing problems - it's about protecting patients and maintaining confidence in your organization.
5 Best Practices for Post-Incident Communication in Healthcare
How to Communicate Effectively in Emergencies
sbb-itb-535baee
1. Assign a Communication Lead and Define the Chain of Command
Supply chain incidents often lead to confusion, making it essential to have a clear plan for communication. The first step? Assign a single communication lead or team to handle all messaging. This ensures consistent information and avoids mixed messages that can leave stakeholders feeling uncertain. By setting up this structure early, you create a solid foundation for clear and unified communication throughout the crisis.
To stay organized, consider using the Hospital Incident Command System (HICS). Tools like HICS Form 207 can help map out your chain of command, while HICS Form 203 is useful for recording role assignments, and HICS Form 205A ensures contact details and communication channels are documented [1]. Physical table tents can display key HICS roles, and Job Action Sheets can outline specific responsibilities. These steps clarify the reporting structure, so everyone knows their role and what’s expected of them. This level of preparation not only improves communication during the crisis but also speeds up recovery efforts.
Your communication lead should have access to real-time data. A cloud-based supply chain dashboard paired with a risk management tool like Censinet RiskOps™ can centralize critical information, keeping the team informed and ready to act. This is especially important considering that nearly 80% of healthcare providers anticipate supply chain challenges will either persist or worsen in the coming year [2].
Lastly, make sure your internal command structure aligns with your community's emergency framework. The Joint Commission emphasizes this in Standard EM.01.01.01, which states: "The hospital's incident command structure is integrated and consistent with its community's command structure" [1]. Using a unified framework ensures smooth coordination with local agencies, making recovery efforts more efficient and effective.
2. Deliver Timely, Transparent Updates to All Stakeholders
Silence during supply chain disruptions breeds uncertainty, which can quickly spiral into mistrust. Whether it's patients, clinical staff, vendors, or community partners, your stakeholders need timely and consistent communication. Delays in updates leave room for assumptions that can damage relationships and make recovery even harder. Clear, structured updates are key to maintaining confidence throughout the process.
Every update should include four essential elements: a brief summary of the incident (including its duration), the root cause, actions taken to address the issue, and steps being implemented to prevent a recurrence. This approach provides stakeholders with the necessary context while avoiding information overload. Tailor your communication - technical teams may need detailed updates, while patients and external partners benefit from concise, empathetic messaging. These tailored updates not only inform but also help rebuild trust as part of your recovery strategy.
When delivering updates, it’s crucial to acknowledge uncertainties without guessing. Be honest about what you know and what you’re still investigating. For example, if the root cause is unclear or you don’t yet have a resolution timeline, say so. Avoid making promises you can’t keep - this honesty, even when the news isn’t ideal, helps establish credibility and reassures stakeholders that you’re being upfront.
Once the issue is resolved, follow up with a thank-you message to your stakeholders, confirming the corrective measures you’ve put in place. This final communication reinforces trust and shows your appreciation for their patience and support during the crisis. Post-incident communication isn’t just about managing the fallout - it’s also an opportunity to strengthen relationships with those who rely on your organization.
3. Create a Communication Plan with Escalation Procedures
Having a documented communication plan ensures that everyone knows who says what, when, and how - eliminating delays during a crisis. This plan should outline key messages, delivery methods, and clear escalation steps, so roles and responsibilities are understood well before any incident occurs. It’s a proactive way to keep communication smooth and effective.
Start by defining the information to be shared at each stage of the incident. This might include an incident summary, a straightforward explanation of the root cause, steps being taken to resolve the issue, and actions to prevent future occurrences. Be specific about which channels to use for different types of updates - such as email for detailed reports, text messages for urgent alerts, and the patient portal for broader public updates. Also, tailor your messaging to suit different audiences, like technical teams versus patients.
Escalation procedures are another critical part of the plan. Specify when and how issues should move up the chain of command. For example, if a vendor delay is likely to affect patient care within 24 hours, senior leaders - like the Chief Medical Officer and Chief Operating Officer - should be notified immediately. Similarly, if there’s a risk of data exposure, the privacy officer and legal team must be involved without delay. Having these thresholds defined ahead of time ensures the communication lead knows exactly when to escalate.
Include a list of support contacts and establish feedback channels for quick follow-up. Setting up a dedicated email address or hotline for incident-related questions can help streamline responses. Assign team members to monitor these channels and respond promptly, reducing confusion and demonstrating your commitment to clear, transparent communication throughout the recovery process.
Make sure the plan is stored in a centralized, easily accessible location, such as an internal wiki, a shared drive, or an incident management platform. This repository should include message templates, escalation flowcharts, and stakeholder contact lists, so your team can quickly access the resources they need. After each incident, update the repository to reflect lessons learned and process improvements. Using platforms like Censinet RiskOps for healthcare can simplify this process, offering a secure and efficient way to manage all communications and updates related to incidents.
4. Review Communication Effectiveness After Each Incident
Once an incident is resolved, it’s important to take a step back and evaluate how well your communication strategy worked. This means analyzing how effectively information was shared and gathering feedback to identify both strengths and areas for improvement. Make it a point to collect input from everyone involved, including internal teams, external partners in the supply chain, and regulators if they played a role. To streamline this, consider adding a feedback link to your final communication so you can capture insights while they’re still fresh.
Use specific metrics to measure communication success. Look at how often inquiries were made and whether certain questions kept coming up - this can highlight areas where key details might have been missed. Stakeholder feedback scores are another great tool to determine if your updates were clear and helpful. Also, consider whether the level of detail provided matched the needs of different groups. For example, technical teams might need in-depth explanations, while clinical staff or patients may prefer simpler, more concise updates.
Centralize and document all communications for future reference. Every acknowledgment, update, and resolution summary should be stored in an easily accessible, searchable location, like an internal wiki or incident management platform. This archive can help you spot patterns over time and improve your response to future incidents. Tools like Censinet RiskOps™ can simplify this process by offering a secure and organized way to manage all incident-related communications.
Go beyond surveys by directly engaging key stakeholders. Reaching out to supply chain partners or department leaders can uncover valuable insights that metrics alone might not reveal. Ask specific questions: Was the root cause clearly explained? Were updates timely? Did they need additional information? These one-on-one conversations often bring to light communication gaps that might otherwise go unnoticed.
Turn insights into action immediately. Update your communication templates to address any issues or confusion identified during the review. For example, if technical jargon caused misunderstandings, revise your language to make it more accessible. If escalation procedures were unclear, refine those processes before the next incident. Make it a priority to update all relevant documentation and templates before officially closing the incident, ensuring the lessons learned are preserved and ready to improve future responses.
5. Update Communication Protocols Based on Lessons Learned
An incident review has real value only when it leads to actionable improvements. Once you've collected feedback and pinpointed what worked and what didn’t, it’s time to revise your communication protocols. This might involve adjusting templates, refining escalation procedures, or updating contact lists to address gaps identified during the review.
Every change should be documented along with the reasoning behind it. For instance, if stakeholders frequently asked about vendor contingency plans during an incident, you should add a section addressing this in future communications. Similarly, if technical jargon caused confusion for clinical staff, update your language guidelines to make communications clearer and easier to understand. These updates should be reflected immediately in your organization’s internal wiki or incident management system.
Don’t wait for annual reviews to implement changes - act quickly after an incident. Prompt updates ensure that lessons learned are applied while they’re still fresh, reducing the risk of repeating past mistakes.
Tailor these updates to suit the needs of different audiences. Internal teams, like IT or supply chain, require detailed breakdowns, including root cause analysis and process adjustments. On the other hand, external partners and patients need clear, empathetic explanations that focus on the incident’s impact and resolution. Using audience-specific templates can save time and prevent misunderstandings in the future.
Store all revised protocols in a centralized, easily searchable location. This repository should include updated templates, root cause summaries, and acknowledgments of changes made. Tools like Censinet RiskOps™ can help securely organize and retrieve this documentation, ensuring everyone can access the latest protocols when needed.
Conclusion
Strong post-incident communication safeguards patient safety and reinforces trust among stakeholders. By implementing these five practices - assigning a dedicated communication lead, providing timely updates, setting clear escalation procedures, evaluating your effectiveness, and regularly updating protocols - you can shift from reactive responses to proactive preparedness during crises.
When the stakes are high, communication is everything. Research shows that communication breakdowns are responsible for over 70% of sentinel events in healthcare. Additionally, poor collaboration among providers can lead to a 1.8-fold increase in patient risk-adjusted mortality and extended hospital stays [3]. These numbers reflect real lives impacted by how well - or poorly - your organization handles crises.
Timely and transparent communication prevents delays and builds trust. Silence can lead to speculation and frustration, creating long-term damage to relationships with patients, families, and other stakeholders.
Each incident is a chance to improve. With every event, you can refine your processes, enhance communication templates, and expand institutional knowledge. Tools like Censinet RiskOps™ make it easier to centralize and access updated protocols, ensuring your team is always equipped to respond effectively.
You don’t have to tackle everything at once - just begin. Even small steps, like adopting one or two of these practices, can make a meaningful difference in protecting patient outcomes and preserving your organization’s reputation.
FAQs
Who should lead communication after an incident?
The communication lead plays a crucial role and should have well-defined responsibilities. Ideally, they are integrated into the incident response team or the broader governance structure. This ensures communication with all stakeholders is coordinated and effective, both during the incident and in its aftermath.
How often should we send post-incident updates?
It's important to maintain a consistent schedule for post-incident updates. For example, during a major incident, updates could be provided every 2 hours, or according to a pre-communicated timeline. This approach keeps stakeholders informed promptly and avoids unnecessary delays.
When should an incident be escalated to executives or legal?
When an incident involves major risks to patient safety, compliance, or legal responsibilities, it should be escalated to executives or legal teams. For instance, a data breach affecting 500 or more individuals or situations causing serious operational or reputational damage often demand high-level decision-making or legal evaluation.


