AI in Consent Revocation Systems
Post Summary
AI is transforming how healthcare organizations handle consent revocation. When patients withdraw consent, their data must stop being shared immediately. Traditional systems rely on manual processes like forms or spreadsheets, which often lead to delays, errors, and compliance risks. In contrast, AI-driven systems automate enforcement, ensuring instant updates across networks. These systems use tools like machine unlearning, cryptographic binding, and real-time notifications to prevent data misuse and comply with privacy laws like HIPAA and GDPR.
Key points:
- Traditional systems: Slow, manual, prone to errors, and lack real-time enforcement.
- AI systems: Automate revocations, ensure immediate compliance, and provide audit trails.
- Compliance: AI systems address legal requirements and reduce risks of non-compliance.
- User experience: Patients get transparency and control; staff benefit from reduced workloads.
AI systems are more efficient and reliable but come with higher implementation costs and complexity. Organizations must weigh these factors against their privacy obligations and operational needs.
1. Traditional Consent Revocation Systems
Traditional consent revocation in healthcare often depends on manual, paper-based processes. When a patient decides to revoke consent, they usually need to submit a written request - this could be a signed form, a letter, or a secure message through a patient portal. Staff then manually process these requests and update the necessary systems [1]. Unfortunately, this manual approach introduces inefficiencies and creates gaps that are hard to ignore.
Automation and Efficiency
One of the biggest shortcomings of traditional systems is their inability to enforce revocations effectively. These systems tend to treat revocation as a routine administrative task, which fails to address the need for active control. As Impact Insights explains:
"Revocation is often misunderstood as an administrative event: update the form, upload the file, and note the change. In integrated care systems, that is nowhere near enough." [2]
In many cases, organizations rely on outdated methods like email chains or static lists to manage revocations [1]. LeadCompliant highlights the issue, stating that "manual compliance processes break down quickly when you are handling thousands or tens of thousands of leads and calls per day" [6]. This results in delays between recording a revocation and actually enforcing it across all systems, leaving room for errors.
Compliance with Regulations
HIPAA grants patients the legal right to revoke consent at any time, provided it's done in writing [1]. However, traditional systems often struggle with what’s known as "downstream lag" - the delay between updating internal records and notifying external business associates [2][1]. This lag poses serious compliance risks because sensitive information may still be shared even after consent has been withdrawn.
Adding to the complexity, organizations are required to maintain detailed documentation for at least five years. This includes timestamped records, disclosure language, IP addresses, and source URLs [6]. Non-compliance can be costly; for instance, the FTC’s Telemarketing Sales Rule imposes fines of up to $50,120 per violation [6]. These challenges can erode patient trust and expose organizations to significant penalties.
User Experience
From a patient's perspective, traditional revocation systems can feel frustrating and opaque. Requests often come through various channels - phone calls, emails, portal messages, or even in-person visits - requiring manual reconciliation across multiple systems [1]. This lack of integration can lead to delays and confusion.
Healthcare staff face similar frustrations. As Solum Health warns:
"A scanned PDF that no one sees during daily work will not protect you. Connect revocation to visible flags, lists, or consent fields." [1]
When revocation records are buried in static notes or uploaded files, staff may unintentionally continue outreach or share data simply because they aren’t aware of the updated status [1].
Scalability and Adaptability
Traditional systems also struggle with scalability. They often rely on binary decision-making - either maintain all prior coordination or halt everything entirely [2]. This rigid approach can lead to unintended consequences, such as missed follow-ups or poor discharge planning, as organizations err on the side of caution to avoid non-compliance.
Moreover, these systems are ill-equipped to meet modern privacy expectations. Patients increasingly demand granular, purpose-specific controls, but traditional workflows often operate on blanket permissions [7]. Without centralized messaging or automated enforcement, healthcare organizations find themselves caught between meeting privacy regulations and managing day-to-day operations effectively.
sbb-itb-535baee
2. AI-Driven Consent Revocation Systems
AI-driven consent revocation systems shift from passive documentation to active, automated enforcement. These systems handle consent revocation as a control event, triggering instant updates across connected platforms. For example, when a patient withdraws consent, AI workflows immediately validate the current consent state, verify cryptographic document hashes (SHA-256), and enforce restrictions before any data leaves the organization [4].
Automation and Efficiency
These systems centralize revocation requests from SMS, email, and patient portals into a single intake queue, solving the issue of scattered manual processes [1]. They automatically categorize and route revocation events, eliminating the need for staff to chase updates. Using push notifications and webhooks, they notify downstream partners and business associates in real time, ensuring compliance across the entire data network without requiring manual follow-up [4]. This automation is a critical component of modern third-party risk management strategies.
AI further enhances efficiency by detecting and redacting Protected Health Information (PHI) before processing. Using OCR and natural language processing, these systems identify sensitive data - like names, addresses, or medical record numbers - and remove it before any transmission occurs [4]. This PHI minimization step safeguards privacy and ensures only essential data is shared, even before consent revocation becomes an issue. The result? Faster processing and stronger compliance with privacy regulations.
Compliance with Regulations
Regulatory compliance demands that consent revocations are enforced through real-time workflow updates [2]. AI systems manage this by treating consent as a versioned state machine with distinct states: active, revoked, expired, or limited [5]. Each transition generates an immutable, cryptographically anchored audit trail, creating tamper-proof records that can withstand regulatory scrutiny for years.
To ensure long-term compliance, these systems use Long-Term Validation (LTV) packages. These bundles include signatures, certificate chains, and timestamps, ensuring that consent records remain verifiable even after certificates expire [5]. As Daniel Mercer, Senior SEO Content Strategist, explains:
"Treat LTV as a preservation requirement, not a nice-to-have. If a consent artifact can't be verified 5 years from now, it is operationally incomplete even if it validates today" [5].
The EU AI Act, effective as of August 2024, introduces a risk-based framework for AI consent management [9]. By August 2026, healthcare organizations working internationally must comply with provisions for high-risk AI systems, making robust consent infrastructure indispensable [9].
User Experience
AI-driven systems also transform the patient experience. Patients gain transparency and control that traditional methods lack. Instead of wondering if their revocation request was processed, they receive clear receipts and real-time confirmations showing that their preferences have been enforced across all systems [4][8]. This level of visibility builds trust, especially since over 90% of patients believe their health data should remain private and unavailable for purchase [1].
For healthcare staff, these systems reduce administrative workloads. AI eliminates the need to manually update outreach lists, track down clarifications, or check static notes before sharing data [1]. Revocation statuses are made visible and actionable directly within the tools staff already use, streamlining daily operations.
Scalability and Adaptability
AI systems go beyond compliance and enforcement to improve long-term operations. Unlike traditional systems that treat revocation as a binary stop signal, AI enables continuity redesign. This means workflows can be adjusted to maintain safe care coordination through lawful, narrower pathways after broad consent is withdrawn [2]. AI reroutes communications and adapts workflows while respecting patient preferences, ensuring uninterrupted care.
Scalability is another key advantage. Whether handling a handful or thousands of revocation requests daily, these systems maintain consistent enforcement without additional staff. They also support granular, purpose-specific controls, allowing patients to revoke consent for certain uses (like AI analysis) while keeping permissions for direct care intact [7]. This flexibility helps healthcare organizations meet both regulatory requirements and patient expectations without overhauling their infrastructure, proving how AI can elevate consent management across the board.
Advantages and Disadvantages
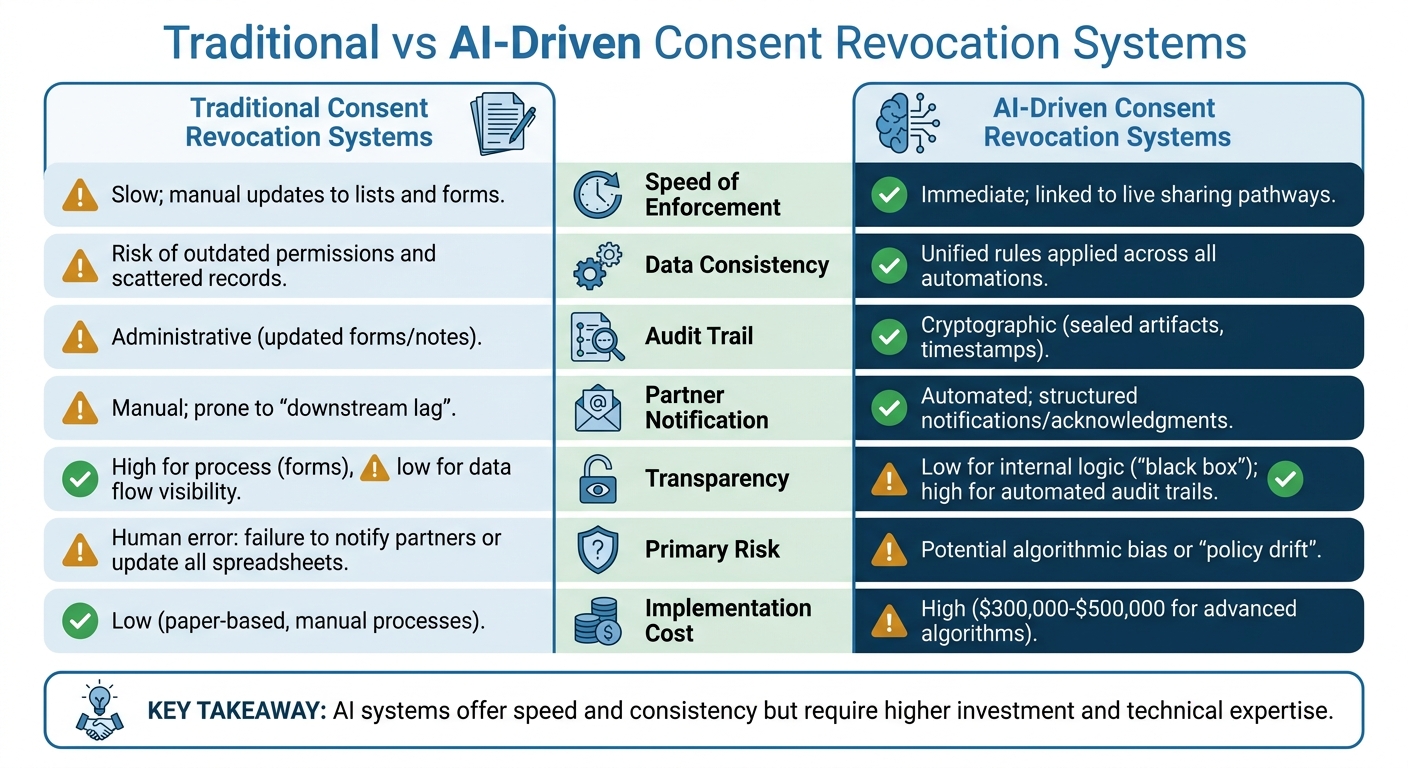
Traditional vs AI-Driven Consent Revocation Systems in Healthcare
Let’s dive into the strengths and challenges of traditional and AI-driven systems, building on the earlier discussion about their functionalities. This comparison sheds light on how each approach handles common issues like outdated permissions and operational efficiency.
Traditional methods are known for their simplicity and familiarity. Patients are comfortable with paper forms, and the process is straightforward. However, these systems often fall short when it comes to keeping permissions up to date. Manual processes can lead to delays in recording revocations, leaving outdated permissions in effect longer than they should be [2].
AI-driven systems, on the other hand, excel in speed and consistency. Revocations are enforced immediately, and secure cryptographic audits ensure machine-verifiable evidence. Traditional systems, in contrast, rely on basic documentation, like a date on a form, which doesn’t provide the same level of defensibility [5]. That said, AI systems come with their own complexity. The "black box" nature of some algorithms can make it hard to explain how decisions are made, potentially complicating the idea of fully informed consent [9].
Scalability is another area where these systems differ. Traditional systems often depend on fragmented tools, like spreadsheets and email inboxes, which become harder to manage as patient volume increases [1]. AI systems are designed to handle large volumes more efficiently, using unified messaging hubs and automation to streamline processes [1]. However, frequent consent prompts in AI systems can lead to "consent fatigue", where users approve requests without proper consideration [9].
Here’s a quick comparison:
| Feature | Traditional Revocation Systems | AI-Driven Revocation Systems |
|---|---|---|
| Speed of Enforcement | Slow; manual updates to lists and forms [2] | Immediate; linked to live sharing pathways [2] |
| Data Consistency | Risk of outdated permissions and scattered records [1] | Unified rules applied across all automations [1] |
| Audit Trail | Administrative (updated forms/notes) [2] | Cryptographic (sealed artifacts, timestamps) [5] |
| Partner Notification | Manual; prone to "downstream lag" [2] | Automated; structured notifications/acknowledgments [2] |
| Transparency | High for process (forms), low for data flow visibility [1] | Low for internal logic ("black box") [9]; high for automated audit trails [5] |
| Primary Risk | Human error: failure to notify partners or update all spreadsheets [1] | Potential algorithmic bias [9] or "policy drift" [5] |
Ultimately, organizations need to weigh these factors against their specific needs, including patient volume, technical resources, and regulatory requirements [2].
Conclusion
Traditional methods handle revocations passively, but AI-driven systems take a more active role, enforcing them across networks in real time.
This shift offers clear advantages. AI systems enable instant enforcement through live controls, unified communication channels, and cryptographic audit trails. A 2023 study demonstrated this potential when researchers used AI-powered "Audit to Forget Software" to successfully remove specific patient data from deep learning models. Impressively, they maintained an accuracy of 0.98 while using only 50–75% of the original training data [3].
For healthcare organizations exploring AI-driven solutions, the first step is mapping existing workflows to pinpoint where revocation requests are overlooked or mishandled. As Stanford Law School wisely notes:
"A disclosure framework is only as strong as the institutions that implement it, and a consent architecture is only as strong as the humans it expects to exercise consent" [10].
To ensure effective consent management, organizations must establish clear accountability for verification processes and partner notifications. Integrating revocation flags into daily operations is also critical.
However, while the technical benefits are compelling, the financial and operational challenges cannot be ignored. Implementing an advanced AI algorithm can range from $300,000 to $500,000 - a significant investment when compared to the risks posed by manual processes that jeopardize patient privacy. Additionally, states like Illinois, Texas, and California now mandate explicit disclosure and consent for AI use in clinical settings [11].
Platforms like Censinet RiskOps™ (https://censinet.com) can help healthcare organizations incorporate AI-driven consent revocation into their broader cybersecurity and risk management strategies. This ensures patient data remains secure at every stage of the process.
FAQs
How does AI revoke consent instantly across all connected systems?
AI takes the hassle out of consent revocation by immediately updating all active information-sharing channels. This means that when a patient decides to withdraw their consent, the system swiftly applies the change across platforms such as case management tools, referral networks, and shared notes. This not only ensures compliance but also reduces delays, keeping everything running smoothly.
What is “machine unlearning,” and when is it needed after consent is revoked?
Machine unlearning refers to the process of erasing the impact of specific data from AI models that have already been trained. This becomes particularly important in healthcare when a patient withdraws their consent for using their data. It ensures that the model no longer retains or utilizes that information, safeguarding patient privacy, adhering to ethical guidelines, and meeting the requirements of data privacy regulations like the GDPR's "Right to be Forgotten."
What evidence do organizations need to prove revocation compliance under HIPAA and GDPR?
Organizations need to maintain clear documentation of patient consent and any subsequent revocations. This means keeping records of written authorizations for non-standard uses, as required under HIPAA, and ensuring that updates to data-sharing practices are promptly recorded when a revocation occurs. This approach helps meet compliance requirements under both HIPAA and GDPR.


